Creating Progress Notes
Progress notes help you document client sessions clearly, efficiently, and in alignment with your practice’s clinical and administrative needs. This article walks through how to create, edit, and complete progress notes in Sessions Health, including adding structured details, managing related clinical information, handling signed notes, and using optional tools like attachments, MSEs, and psychotherapy notes.
💡Looking for a quick way to start? To complete a progress note quickly, open the appointment, enter your documentation, and select Sign and Complete. You can explore the additional tools and workflows below as needed.
In this article:
- Video Tutorial
- Adding a Progress Note to a Client Session
- Editing Progress Notes After Signing
- Supervision and Signing Off on Client Notes
- Adding Attachments to Progress Notes
- Updating Medications
- Adding a Mental Status Exam (MSE)
- Managing Diagnoses from Progress Notes
- Updating Treatment Plan Progress
- Adding Psychotherapy Notes
- Frequently Asked Questions
- Related Resources
Video Tutorial
A full demonstration of opening, editing, and completing a progress note.
Adding a Progress Note to a Client Session
Use this workflow to document a session directly from your schedule, the client chart, or your Home page.
Steps to Complete a Progress Note
- Open the appointment.
- From Home > Needs Attention > Incomplete Notes
- From the Calendar by selecting the Note icon
- Solid icon indicates a completed note
- Outline icon indicates an incomplete note
-
From the Client Chart > Summary tab or under Needs Attention on the right-hand column
-
Choose or confirm the note template type.
- Enter your session documentation.
- Type directly into the editable fields provided by the template.
-
Use the formatting toolbar to apply bold, italics, headings, or lists.
-
Add optional details (see steps below).
-
Select Sign and Complete when the entire note is complete.
- In the pop-up, confirm your signature, then select Sign and Complete.

Switching Note Types
You can quickly choose between your enabled templates by selecting the drop-down at the top of the Notes section. Progress Note templates can be added, edited, or removed from Forms & Documents > Forms > System Forms or My Forms.
ℹ️ Switching templates after you’ve started a note triggers a warning. Select Cancel to keep your content or Continue to clear it.
Using Load Last Note
Using the Load last note button helps you document sessions more efficiently by pulling in the previous note of the same type for that client. After selecting your template, choose Load last note to populate the fields with your prior entry so you can update only what has changed instead of starting from scratch.

Editing Progress Notes After Signing
Signed progress notes are locked to protect the clinical record. Most edits require unlocking the note, but you can update the session’s start and end times without unlocking. Use the workflows below depending on what you need to change.
Unlocking a Progress Note
Unlocking allows you to edit all fields in the note, including the template content, attachments, diagnosis, and treatment plan.
-
Open the signed note from Home, the Calendar, or the Client Chart.
-
Select Unlock.
-
Make your changes.
-
Re‑sign the note to complete the update.

Editing Session Times
You can update the session’s start and end times on a signed note without unlocking it. This exception exists because time corrections are often administrative rather than clinical, and adjusting them does not change the clinical content of the note.
-
Open the signed note from Home, the Calendar, or the Client's Chart.
-
Select Edit Times. This option appears only on signed notes.
-
Update the Start Time and End Time fields in the Edit Times window.
- Select Save.
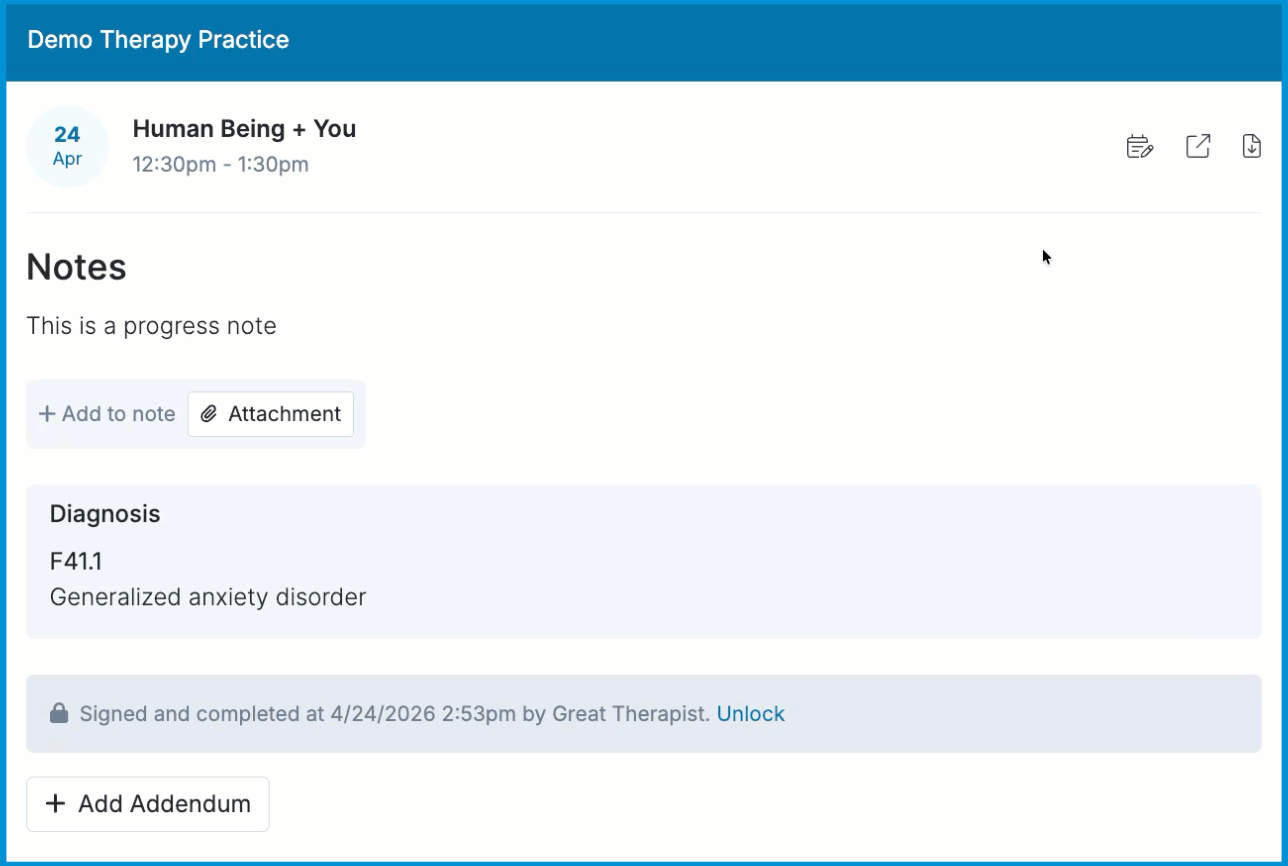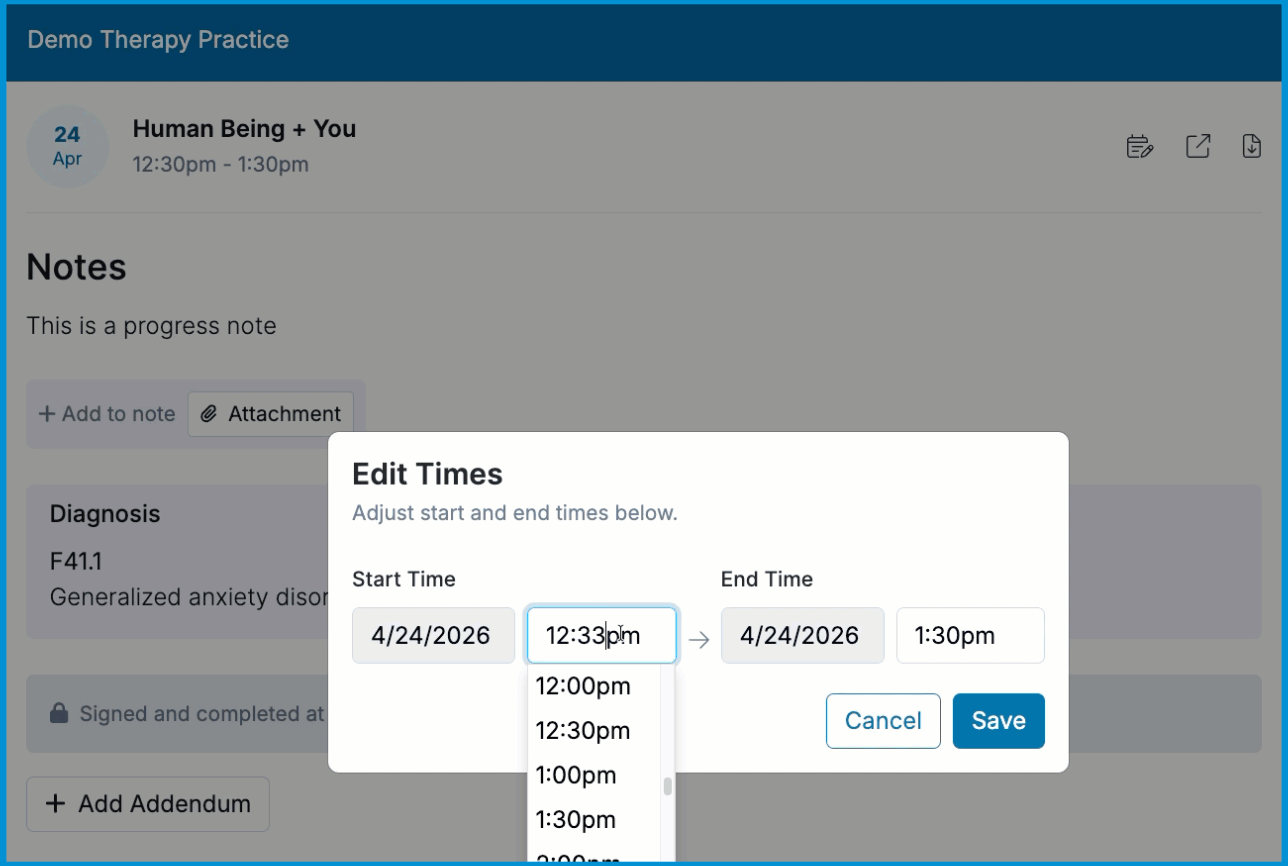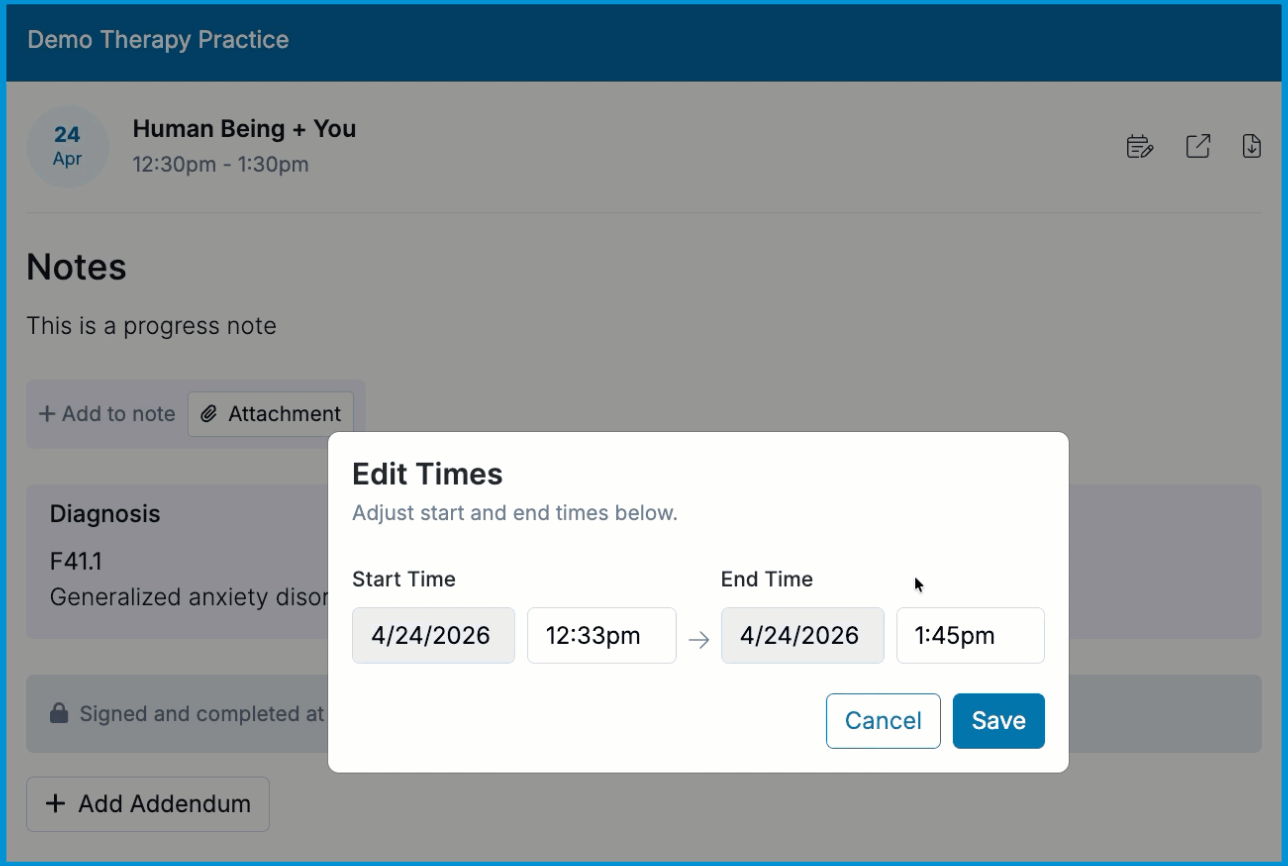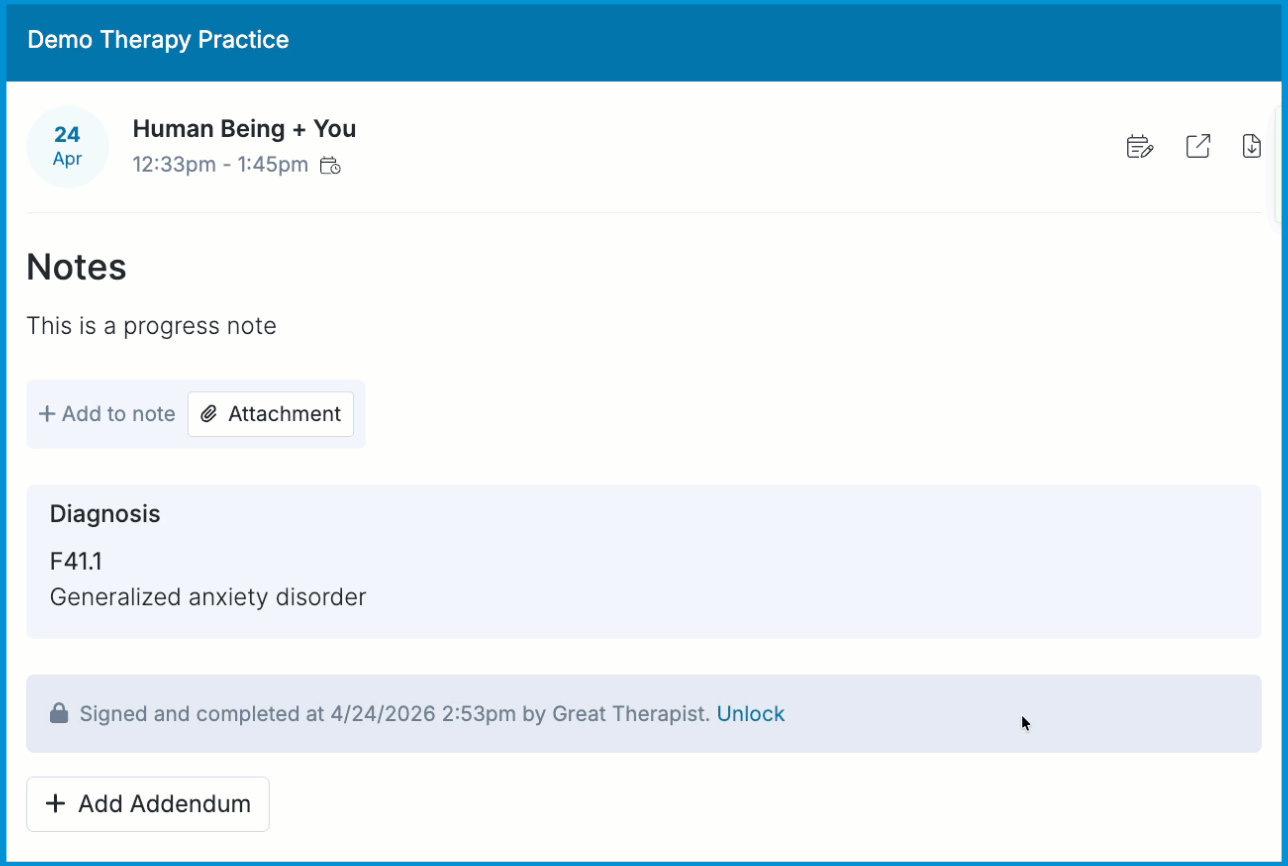
ℹ️ You can only edit the start and end times while the note is locked. All other changes require unlocking the note, and the Edit Times option may not appear if the appointment is tied to a billing or claim workflow that prevents time updates.
Adding Addendums
You can add an addendum to a signed progress note when you need to include additional information without unlocking or altering the original content. Addendums are added to the note and become part of the clinical record. For full details on how addendums work and when to use them, see our Addendums to Progress Notes article.
Supervision and Signing Off on Client Notes
If a practitioner is assigned a supervisor, signed progress notes may require review before they are considered complete. When a supervised practitioner signs a note, the note will show that it is awaiting supervisor review, and the supervisor will see a task on their Home page under Needs Attention for the pending co‑signature.
ℹ️ For full guidance on how supervision works in Sessions Health, see the Supervision: Notes and Treatment Plans article in the Help Center.
Adding Attachments to Progress Notes
Attachments allow you to include supporting documents, such as recordings or assessments, directly with the progress note.
Steps to Add Attachments
-
Open the appointment and scroll to the + Add to note panel.
-
Select Attachment.
-
Upload your file by clicking Upload Attachment or drag and drop the file into the pop-up. Sessions Health supports a wide range of file types, with a maximum file size of 100MB.
- Select Upload.

Updating Medications
Sessions Health makes it easy to add medications to your clients' records. Medication updates made from a progress note sync directly with the client’s chart.
Steps to Add Medications
-
Open the appointment and scroll to the + Add to note panel.
-
Select Medications.
- Enter or update the client’s medications. Your changes save automatically when you click out of the text box.

Adding a Mental Status Exam (MSE)
The Mental Status Exam helps you document clinical observations consistently within a progress note. You can add an MSE from the Add to note panel at the bottom of the note.
Steps to Add a MSE
-
Open the appointment and scroll to the + Add to note panel.
-
Select Mental Status Exam.
-
Complete the MSE fields. You can set all items to All within normal limits by selecting the checkbox.
-
Add any custom observations as needed. If you enter your own items, separate each one with a comma to add it. Custom entries do not carry over to the next session note.
- Your content is saved automatically.

Managing Diagnoses from Progress Notes
You can review and update a client’s diagnoses directly from a progress note, and any changes you make carry over to the client’s chart. This keeps the diagnosis list consistent across documentation, billing, and treatment planning.
ℹ️ For full guidance on adding, editing, and managing diagnoses, see the Diagnosis and Treatment Plans article.
Updating Treatment Plan Progress
The Treatment Plan section of a progress note lets you review active goals and objectives and record progress as part of your session documentation. If the client has an active treatment plan and the template uses integrated goals, the objectives will appear automatically in the note. Any updates you make here carry over to the client’s chart. If the client does not have an active plan, you can select Set up to create one.
ℹ️ For complete guidance on creating, updating, and managing treatment plans, see the Diagnosis and Treatment Plans article.
Adding Psychotherapy Notes
Psychotherapy notes, sometimes called process notes, allow you to record sensitive clinical reflections that should remain separate from the main progress note. Psychotherapy notes are visible only to you and to practitioners or supervisors with access to the client’s chart. These notes are stored privately and are not included in exports or shared with clients.
Steps to Add a Psychotherapy Note
-
Open the appointment and scroll below the signature section.
-
Select Add Psychotherapy Note.
-
Enter your private notes. The text auto‑saves as you type.
- Select Done.

ℹ️ Some U.S. states treat all written content about a client as part of the clinical record, including psychotherapy notes, so be aware of the laws that apply in your location.
Frequently Asked Questions
How do I customize interventions and mental status exam options?
Sessions Health includes a wide range of built‑in options for interventions and Mental Status Exam fields. You can also add your own items by typing them into the dropdown and pressing a comma to save each entry. Custom items do not persist across notes at this time, but you can add them as needed.
Does your platform offer dictation?
Sessions Health does not include a built‑in dictation tool, but most devices support native speech‑to‑text. If you have a PC, you may click the Windows button + H to launch speech services. If you have a Mac, follow the instruction in this Dictate messages and documents on Mac article. If you have an iPhone, see this Dictation text on iPhone article.
Do you offer e-Prescribing, prescribing, eprescribing, or prescription features?
No. Sessions Health does not currently support e‑prescribing or lab ordering, but new features are added regularly, and this may be available in the future.
Do you have a discharge summary template?
Yes. You can use the Discharge or Termination of Services system template or customize it. You can also create your own template and select it when creating a Clinical Note from the client’s Summary tab. Please see this Custom Forms video tutorial for details on creating your own forms.
Why did I see confetti after finishing my notes?
When you complete your last outstanding progress note, Sessions gives you a small celebration: a quick confetti animation and a friendly toast message. It’s just a little encouragement for getting caught up!
Related Resources
For more guidance on related documentation workflows, explore the resources below:
