Diagnosis and Treatment Plans
Diagnoses and treatment plans are central to clinical documentation in Sessions Health. This article explains how these tools work together, including managing diagnoses, creating and updating treatment plans, and tracking progress toward goals within your session documentation.
In this article:
- Adding a Client's Diagnosis
- Updating a Diagnosis for a Particular Session
- Delete a Diagnosis from the Client Summary Tab
- Creating a Treatment Plan
- Recording Progress Towards Objectives
- Updating a Treatment Plan
- ICD-10 and DSM-V
- FAQ
- Related Resources
Adding a Client's Diagnosis
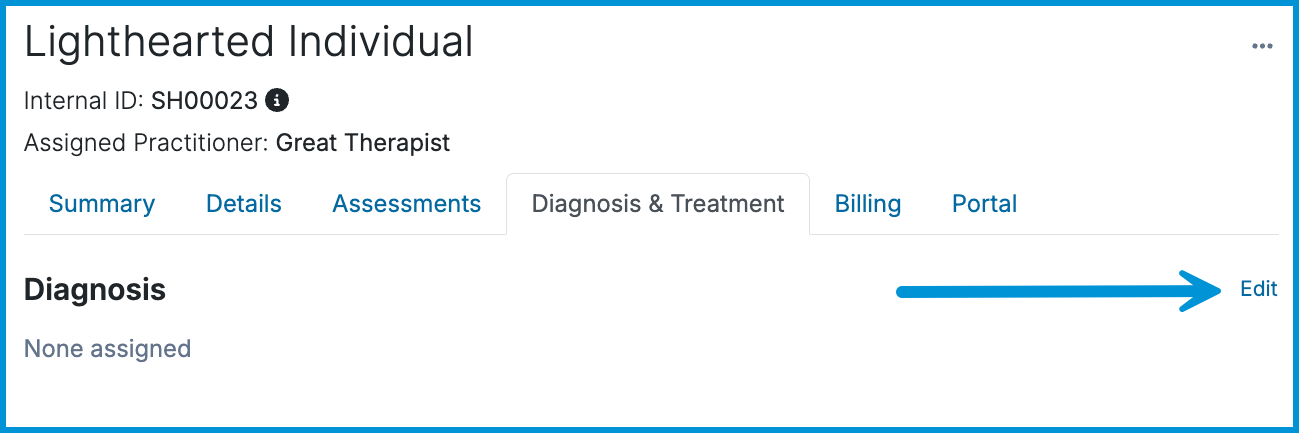
You can manage your client's diagnoses under the Diagnosis & Treatment tab. Start by clicking Edit in the Diagnosis section.
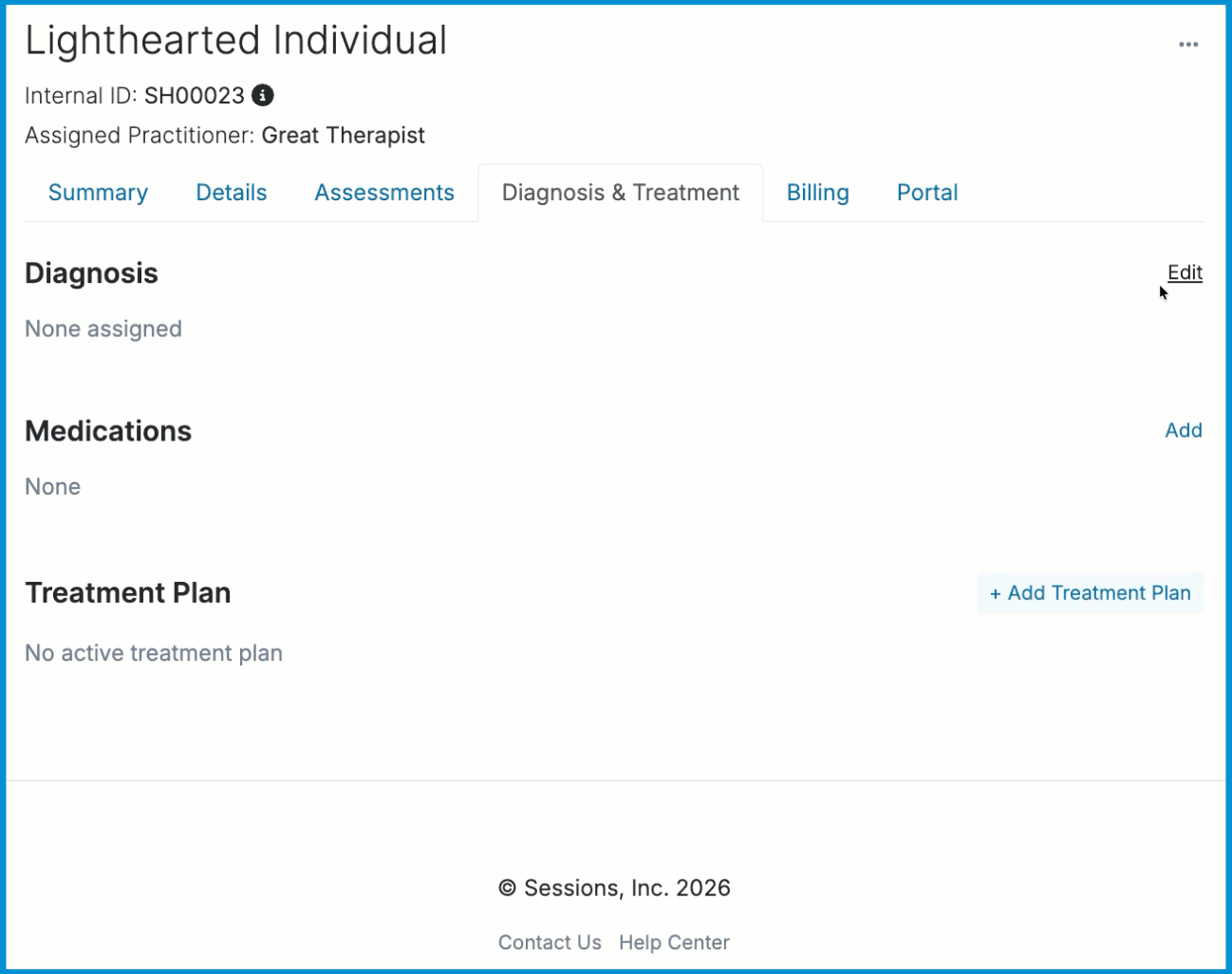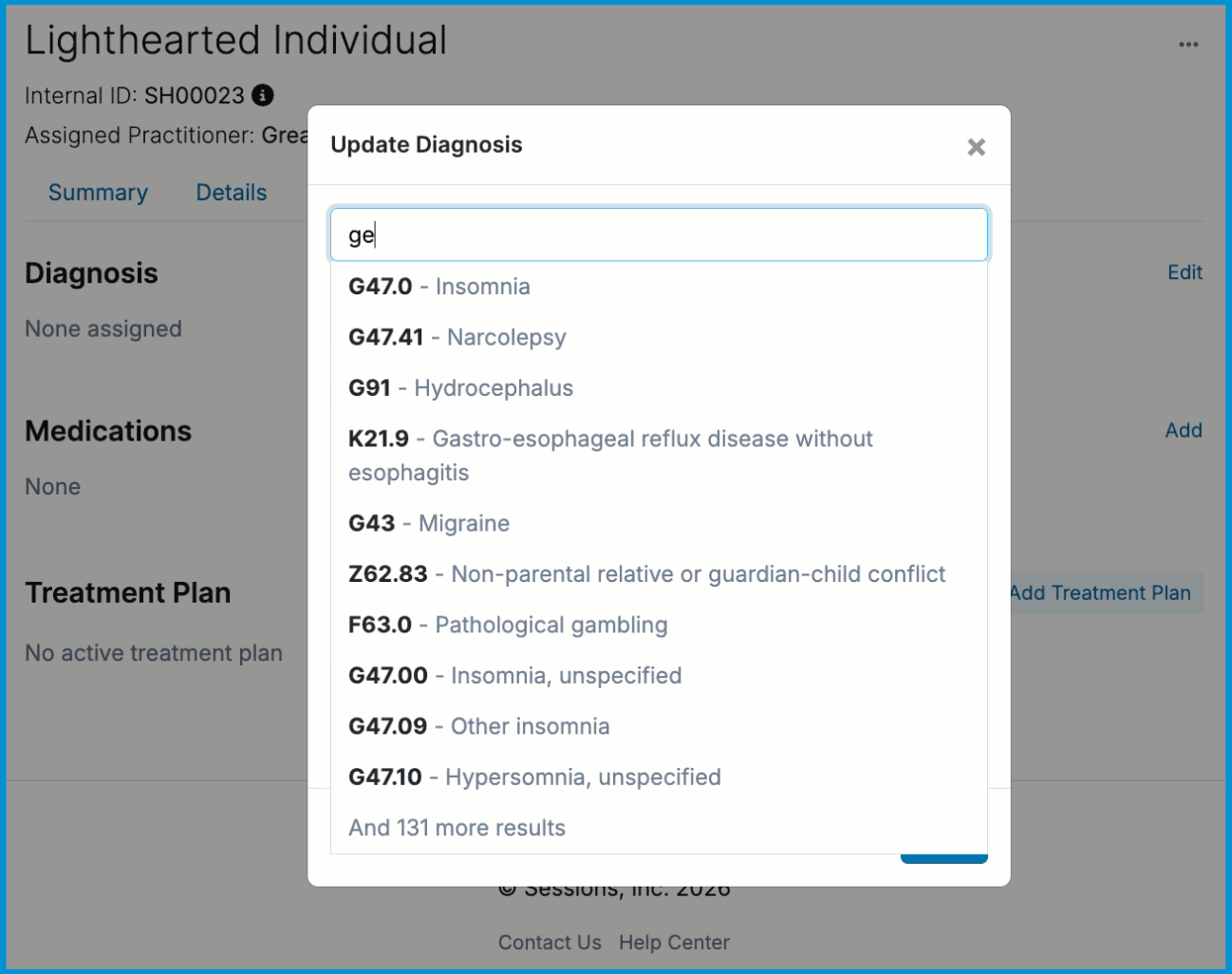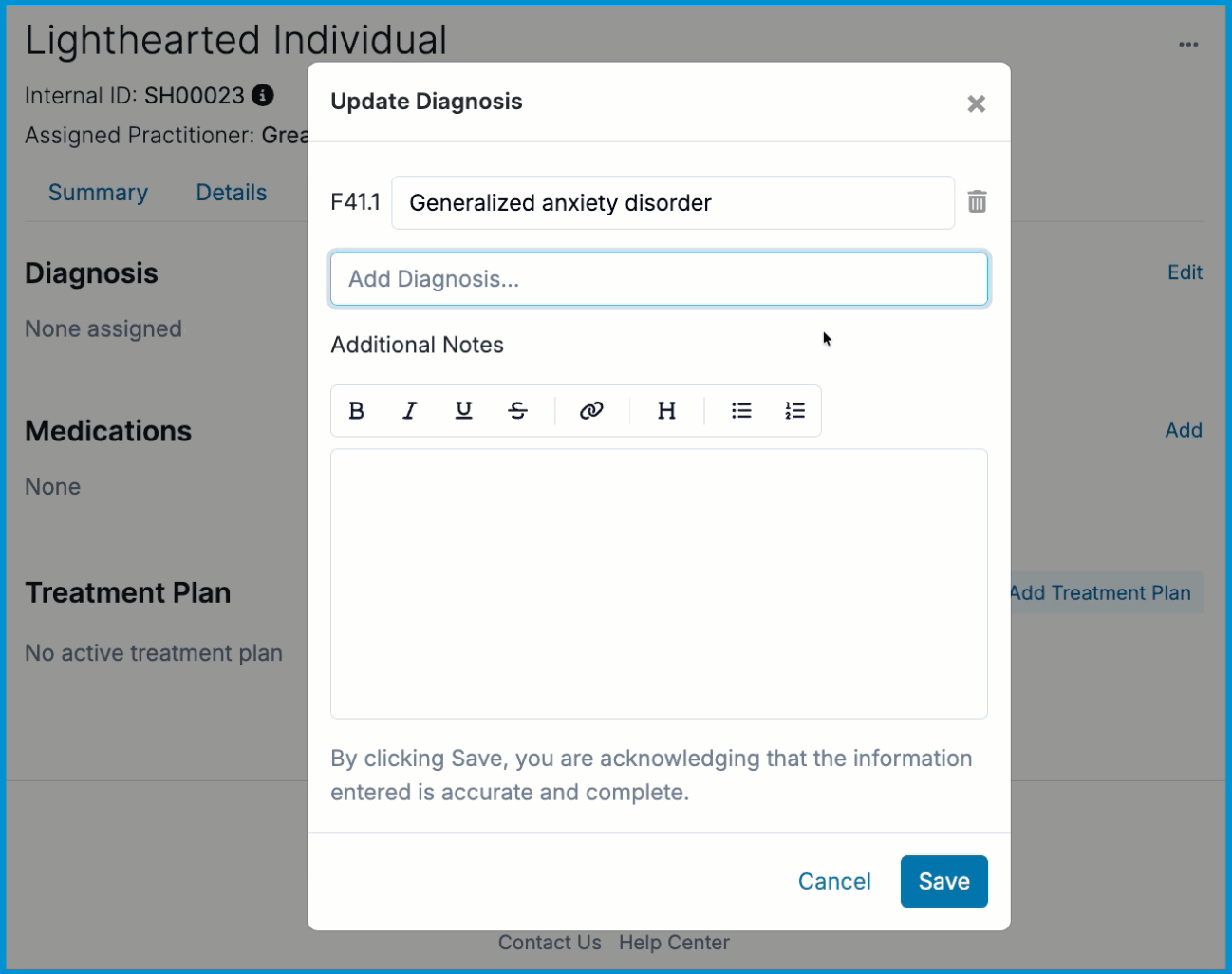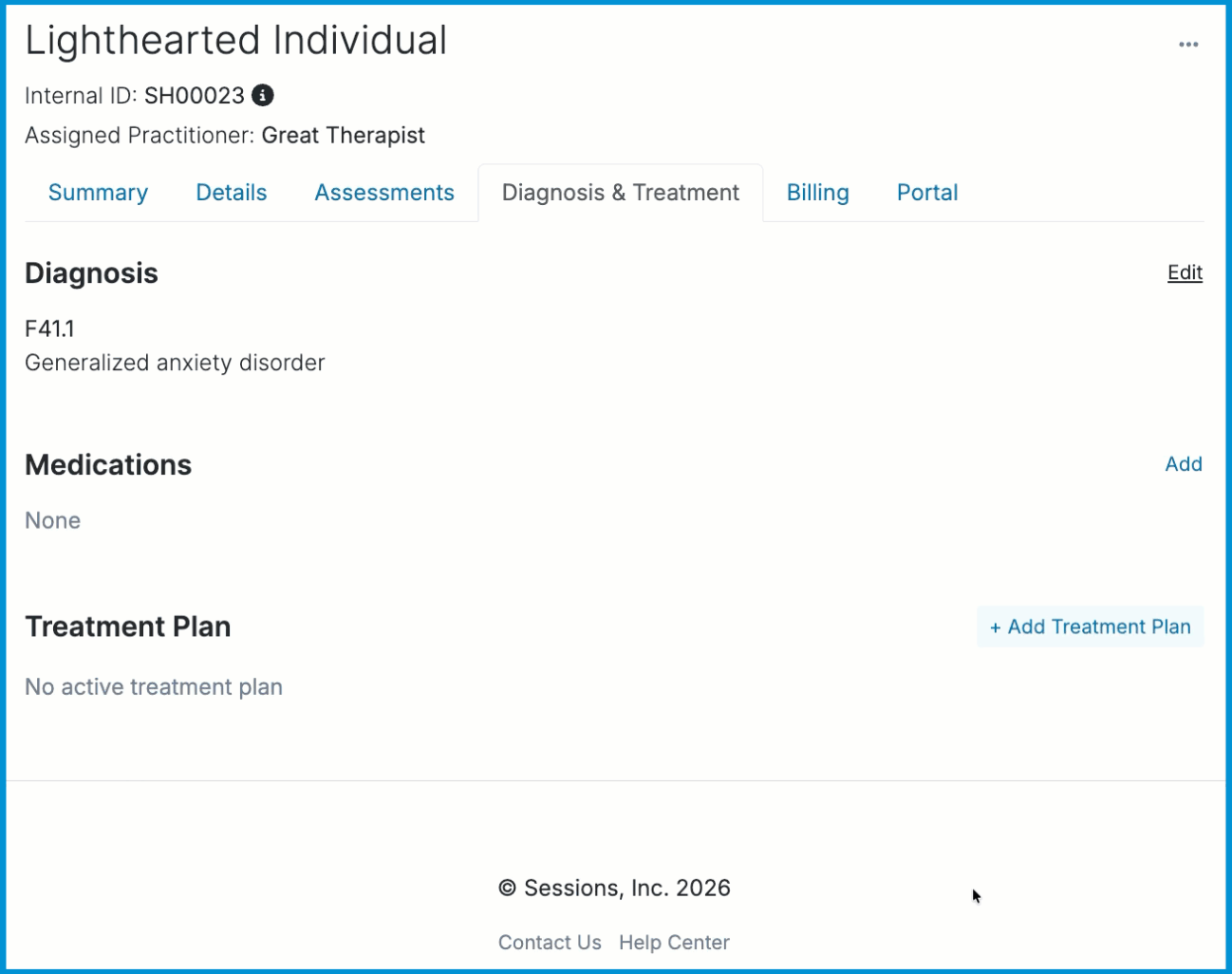
A text field will appear where you can enter an ICD-10 code or diagnosis description. As you type, suggested diagnoses relevant to your input will automatically appear. Select the preferred ICD-10 diagnosis code and description. You can add multiple diagnosis codes at once. Once you click the Save button, the diagnosis code(s) will be added to the client's chart.
ℹ️ Updates to a client's diagnosis will be logged under the client's Summary tab. You will also have the ability to change the client’s diagnosis at the top of any session notes page.
Updating a Diagnosis for a Particular Session
Diagnoses are time-stamped so that if a diagnosis changes over time, each session reflects whatever the diagnosis was at that time. From the note, you can update the diagnosis so that any future documents associated with that session reflect the updated diagnosis.
ℹ️ Any existing documents (e.g. superbill, claim, note) will retain the originally assigned diagnosis that was present at the time the session note was signed and completed.
Customizing Diagnosis Labels
When adding a diagnosis, you may customize the label to suit your approach and/or add modifiers and other information not present by default in the description.

Adding Non-ICD Diagnosis
We can support a general "(other)" diagnosis code. When used, you'll be required to add a custom description.
These custom diagnosis codes will be suppressed from all superbills and claims since we have no method to check their validity. If you want a diagnosis code for claims or superbills that isn't listed in our default options, please contact us at support@sessionshealth.com to add it.
Step 1.
Search for other as a diagnosis.

Step 2.
Enter your description.
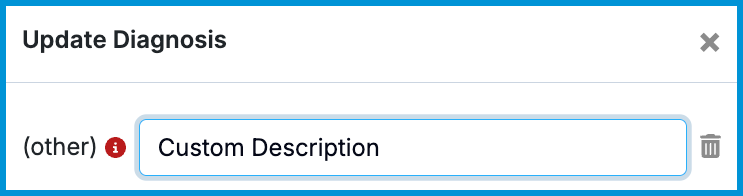
ℹ️ The system will alert you via a red tooltip that the Other diagnosis label is non-billable.
Delete a Diagnosis from the Client Summary Tab
If you accidentally add a duplicate diagnosis or need to remove an entry from the client’s Summary tab, you can delete it.
💡 Removing a diagnosis from the Summary tab does not remove it from the client's chart.
Step 1.
Go to the client’s Summary tab.

Step 2.
Locate the diagnosis you want to remove in the Notes section.
Step 3.
Click the menu icon next to the diagnosis and select Delete.
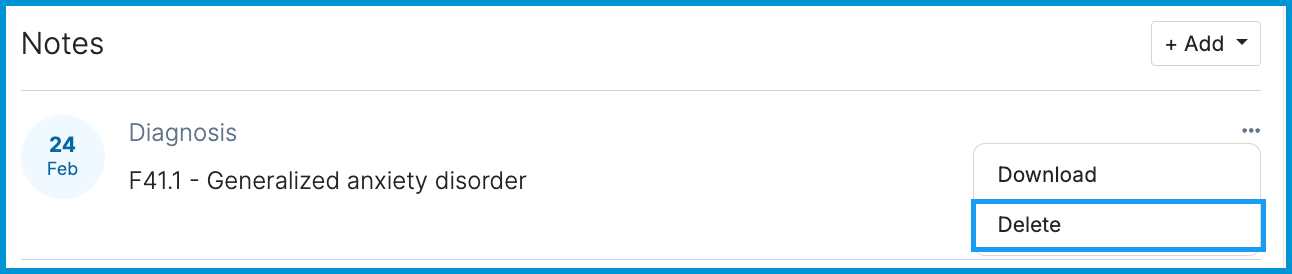
Step 4
Click Delete to confirm.

ℹ️ Deleting a diagnosis from the Summary cannot be undone. Be sure you are removing the correct entry before confirming.
Creating a Treatment Plan
Within a client's Diagnosis & Treatment tab, click the Add Treatment Plan button. You are then presented with two treatment plan options. The Default option offers a standard approach to treatment plans, whereas the Simple option provides a simple text box for you to record your treatment plan.
Creating a Standard (Default) Treatment Plan
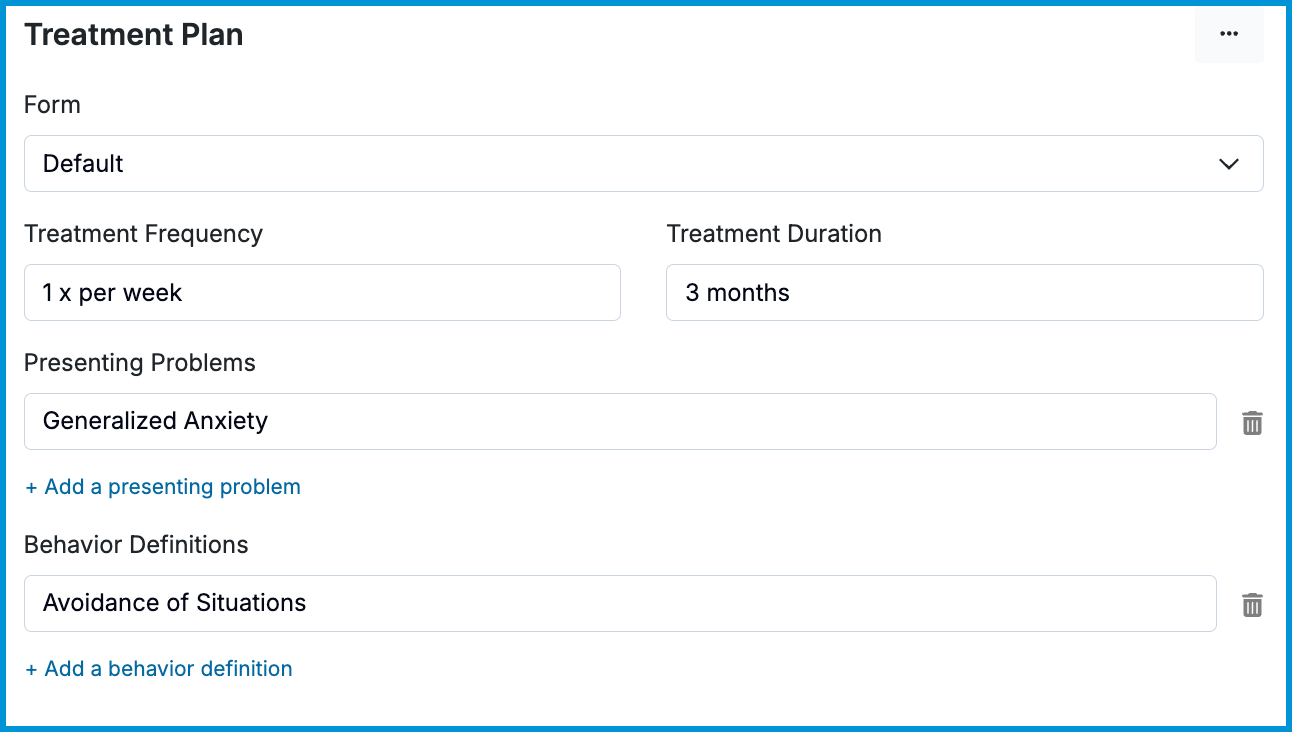
The standard treatment plan will allow you to add presenting problems, behavioral definitions, treatment frequency and duration, and add goals with objectives.
- Presenting Problems: Record what problems led the client to seek treatment.
- Behavior Definitions: Record how have the problems above been affecting your client's day to day life.
- Treatment Frequency: A recommendation for frequency of client sessions.
- Treatment Duration: A recommendation for how long the client should receive treatment.
- Goals: General statements of what the client wishes to accomplish through treatment. You may establish multiple goals within a treatment plan.
- Objectives: These are the building blocks of goals, so are smaller and perhaps, more short term. This could be a specific skill or outcome the client is trying to achieve. You may setup multiple objectives within a goal.
- Interventions: Techniques or treatment modality the therapist will use during the session in order to accomplish objectives. You may choose from a list of drop-downs or type in your own interventions.
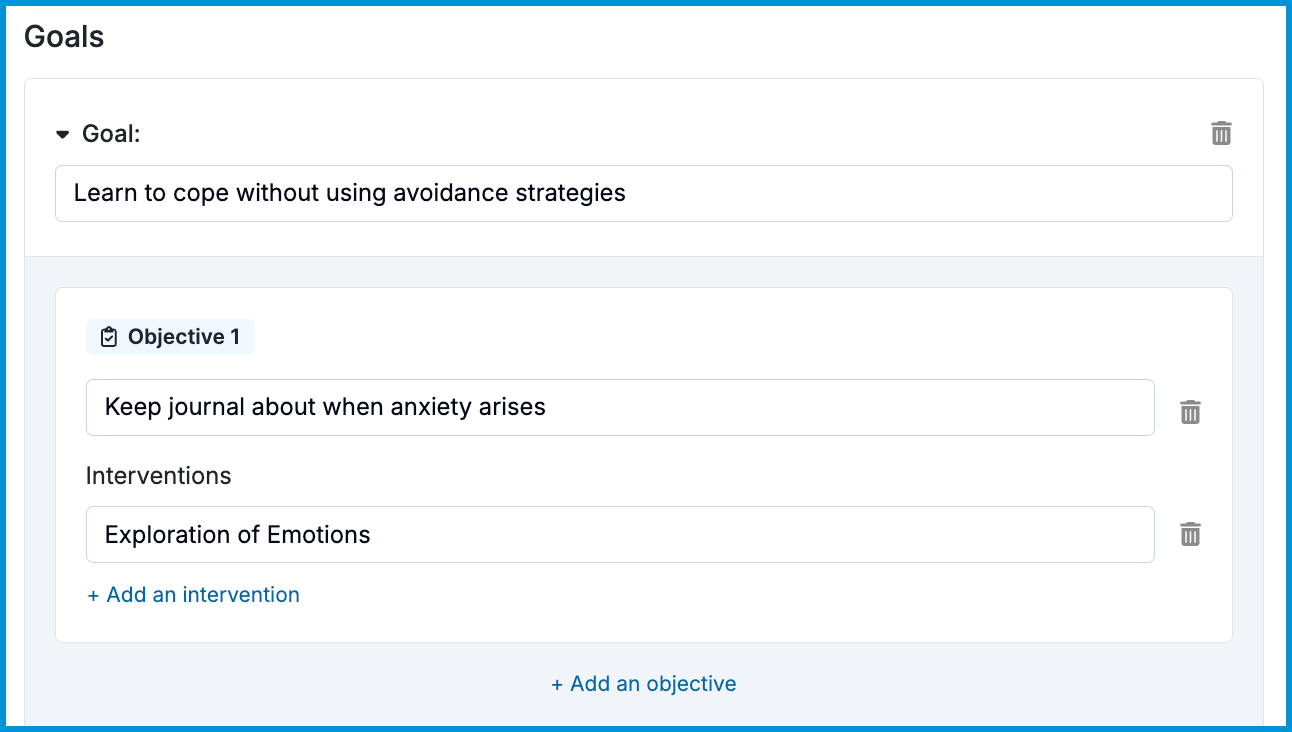
💡 Once you record a goal or objective for one client, those will be saved as options when completing goals and objectives in treatment plans for other clients.
Creating a Custom Treatment Plan
You may create a custom treatment plan with or without the integrated goals, objectives, and interventions from your Forms & Documents > Forms > My Forms page. See our Creating a custom form article on setting up custom forms. Once a custom form is created, it'll appear as an option in the Form drop-down list.
Creating a Simple Treatment Plan
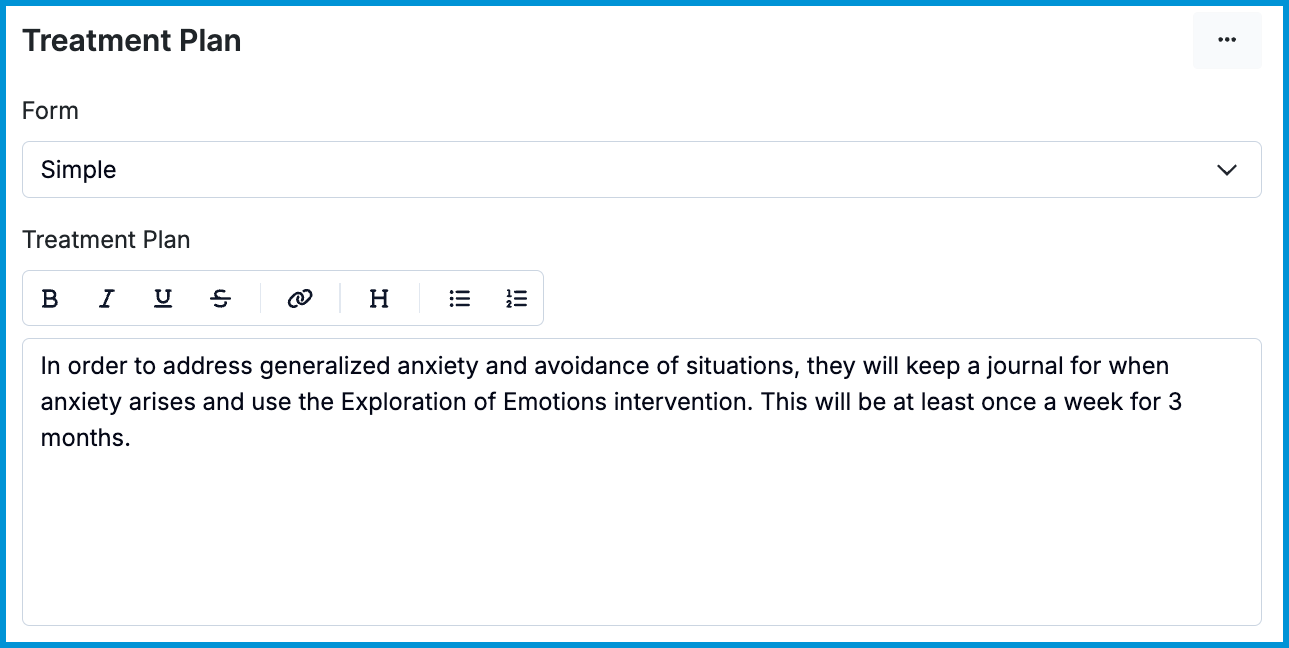
When choosing a Simple treatment plan, a text box will appear for your to record your treatment plan in a single text box. This is helpful if you're copying the treatment plan from a different system or location that doesn't conform to our standard treatment plan template.
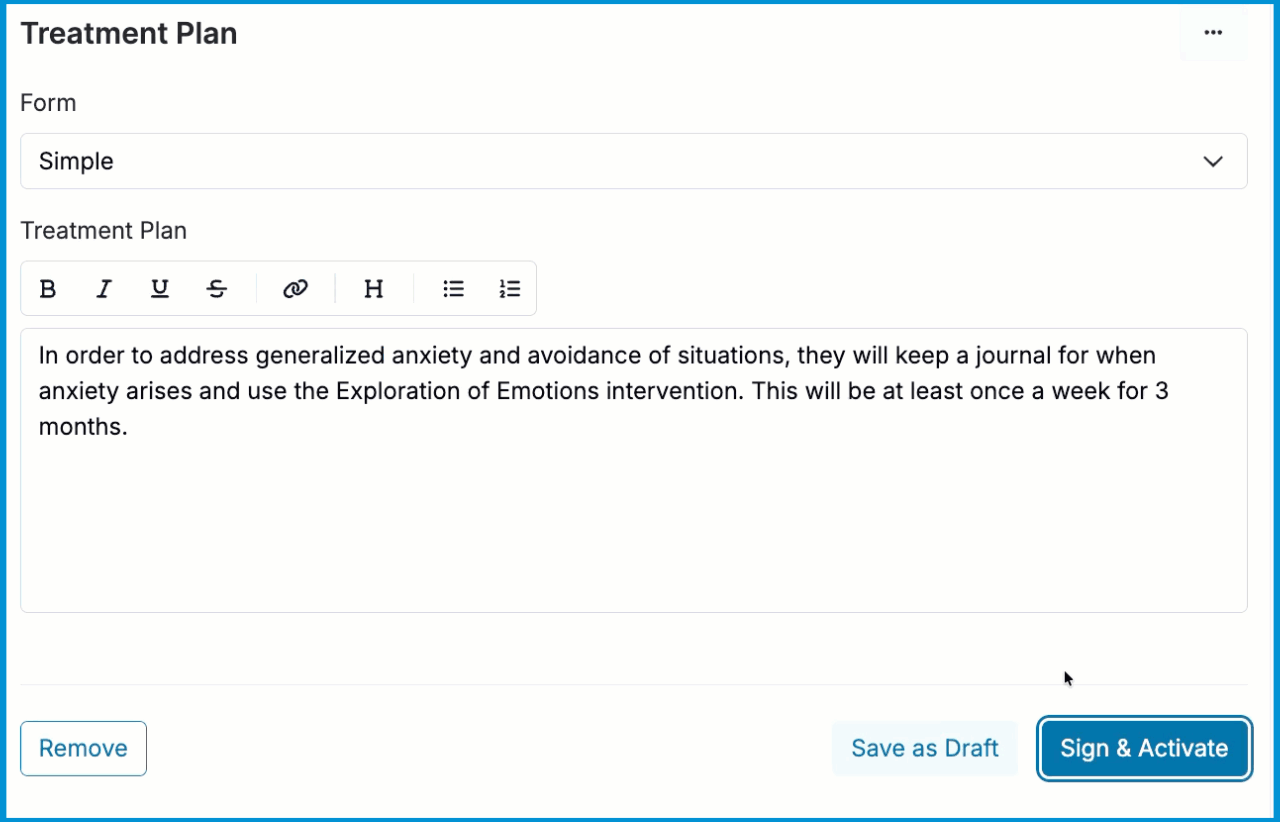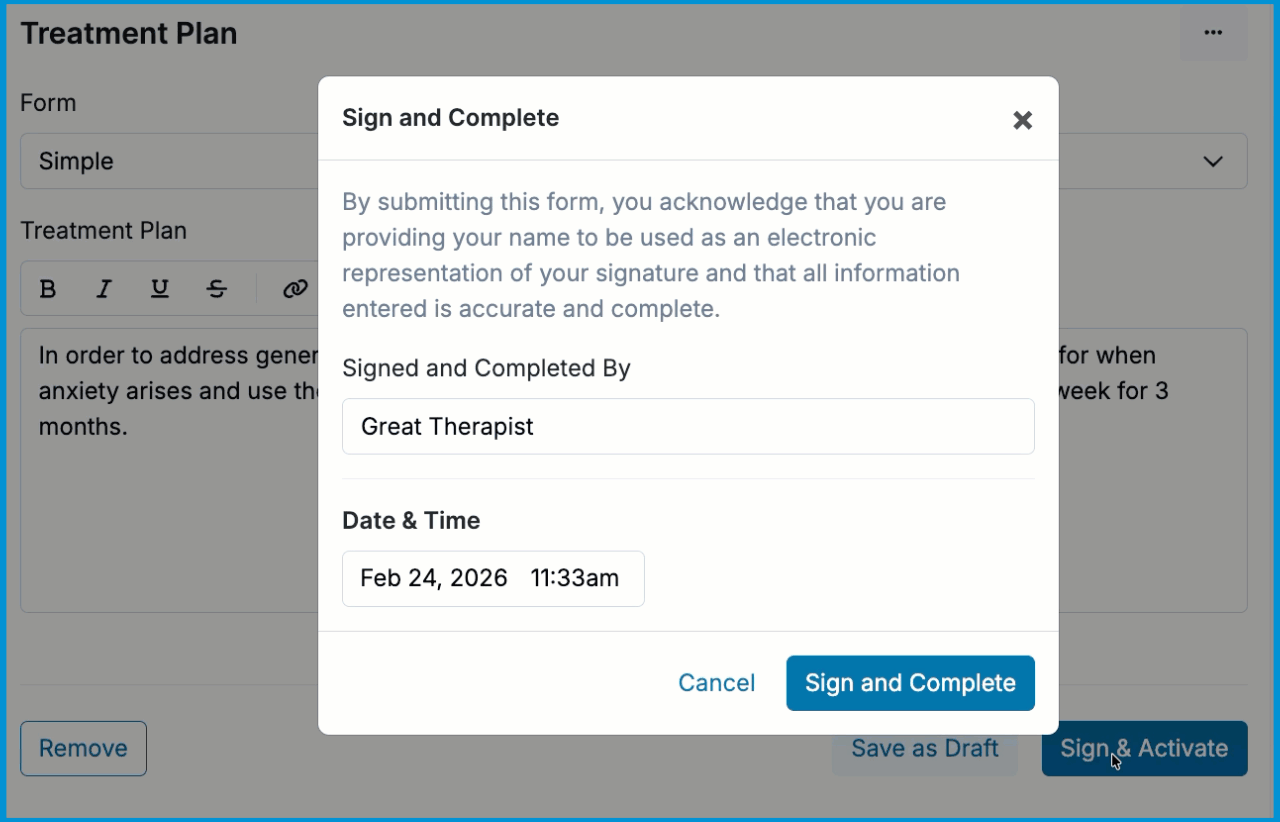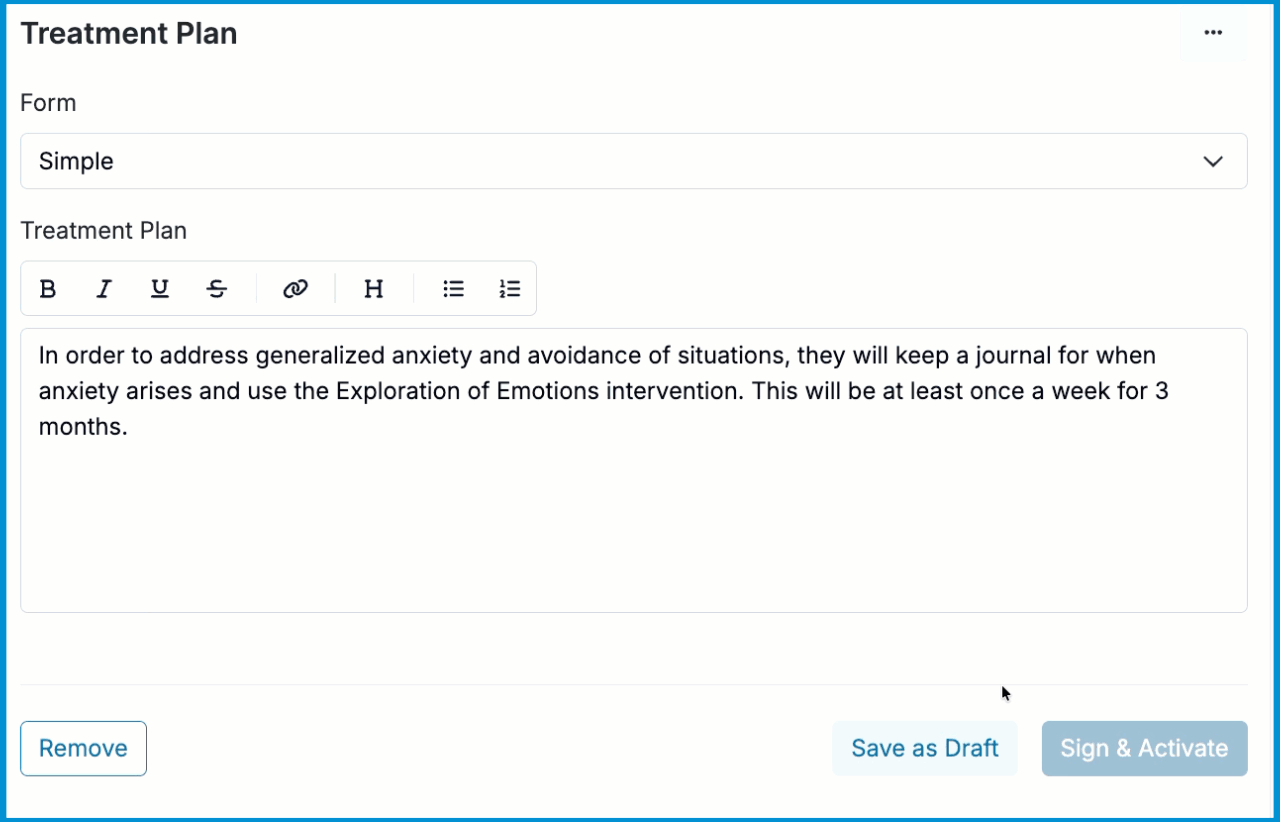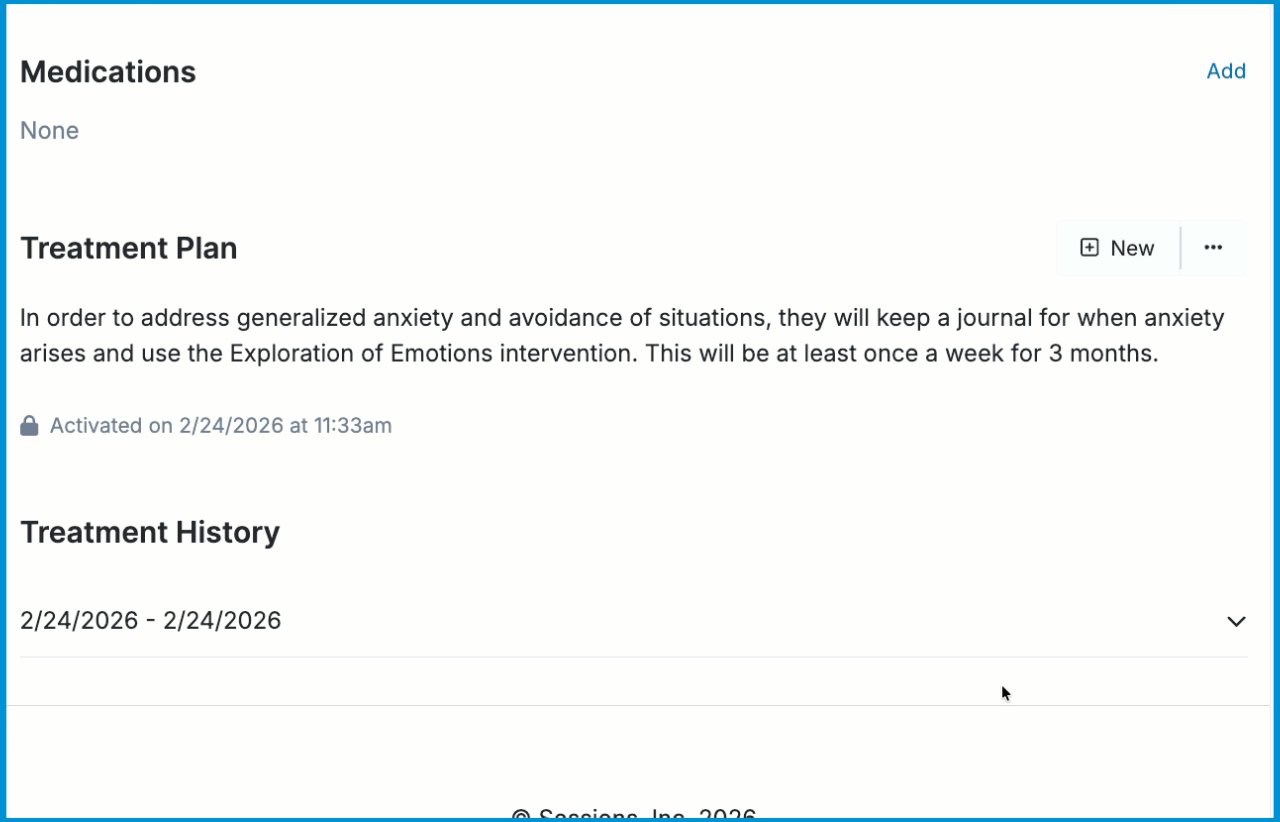
Activating the Treatment Plan
Once your treatment plan is complete, click the Sign & Activate button which will appear highlighted in blue. You will then be prompted to sign the treatment plan.
When an objective is complete, you may return to the Diagnosis and Treatment page and check the box next to the completed objective. The completed date will be recorded in the treatment plan.

Setting Up a Reminder to Review and Update Your Treatment Plan
If you'd like to set up a reminder for yourself to update the treatment plan, click the "..." menu in the top-right corner of the Treatment Plan section. Then, under the Set up Reminder section, you will have the option to select 3 months, 6 months, 1 year, or a custom future date for the reminder. The reminder will appear in the Needs Attention area of your Home page 7 days prior to the reminder date.
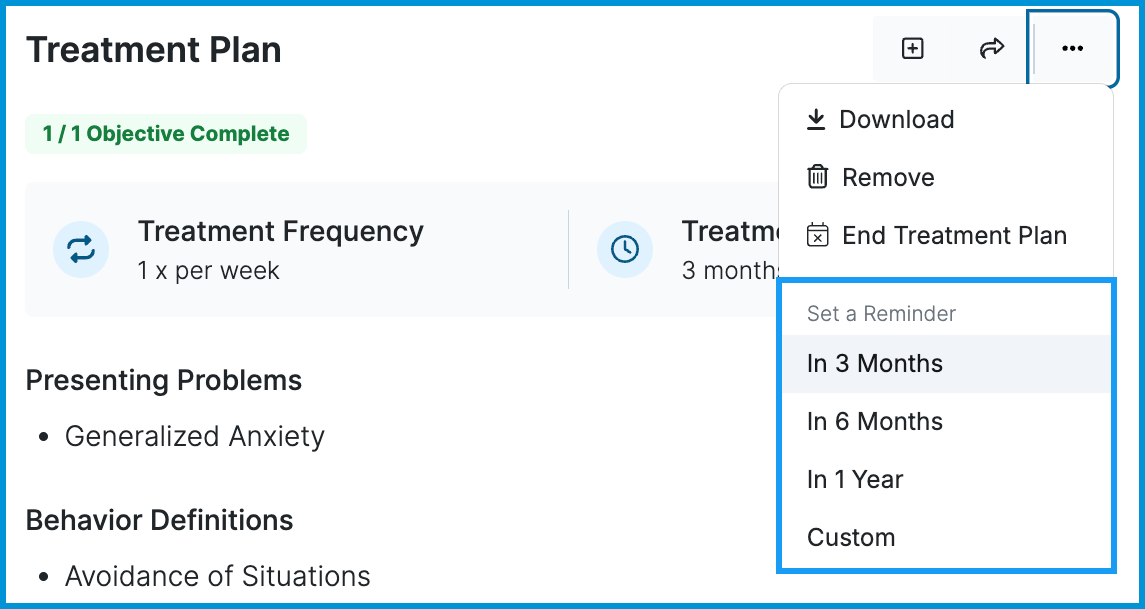
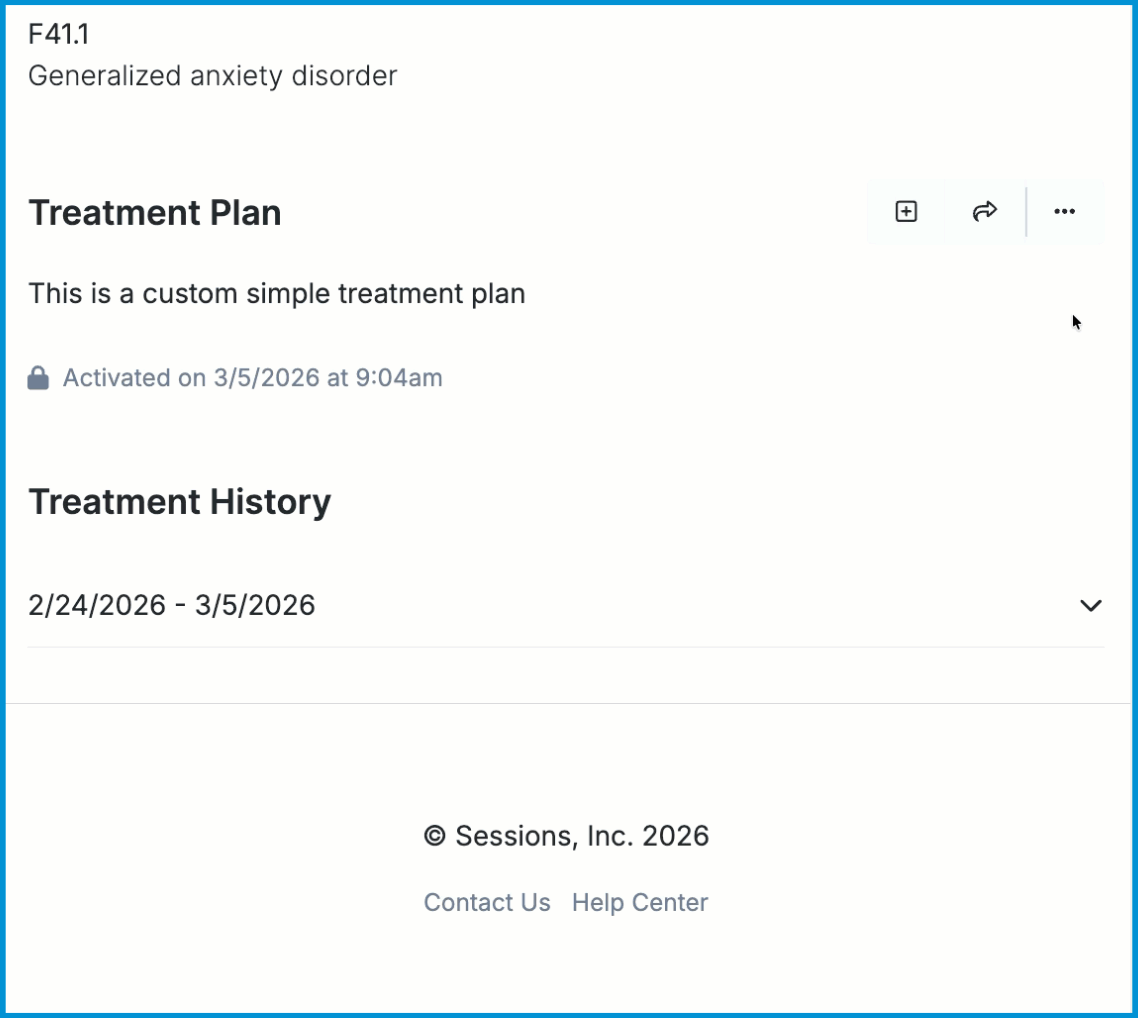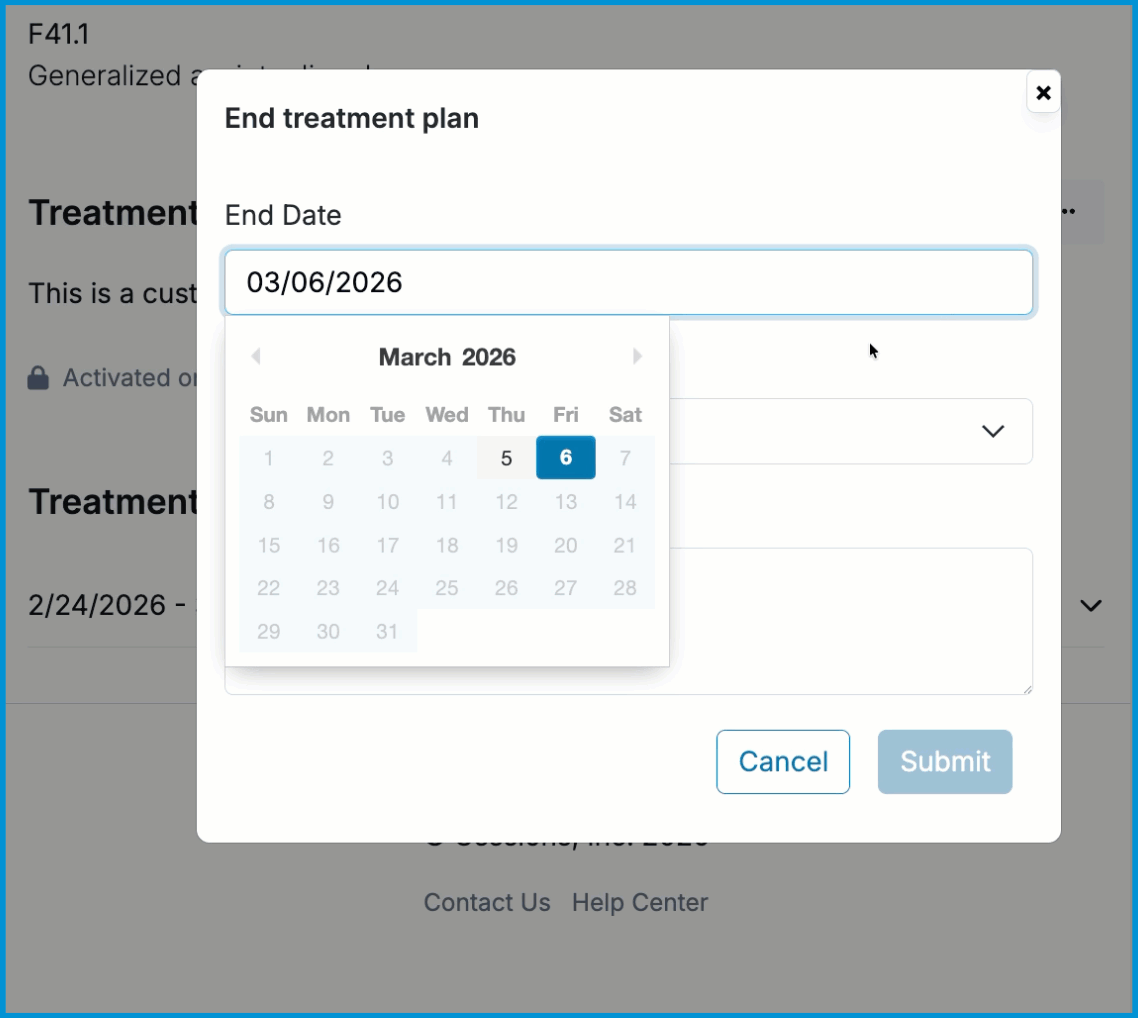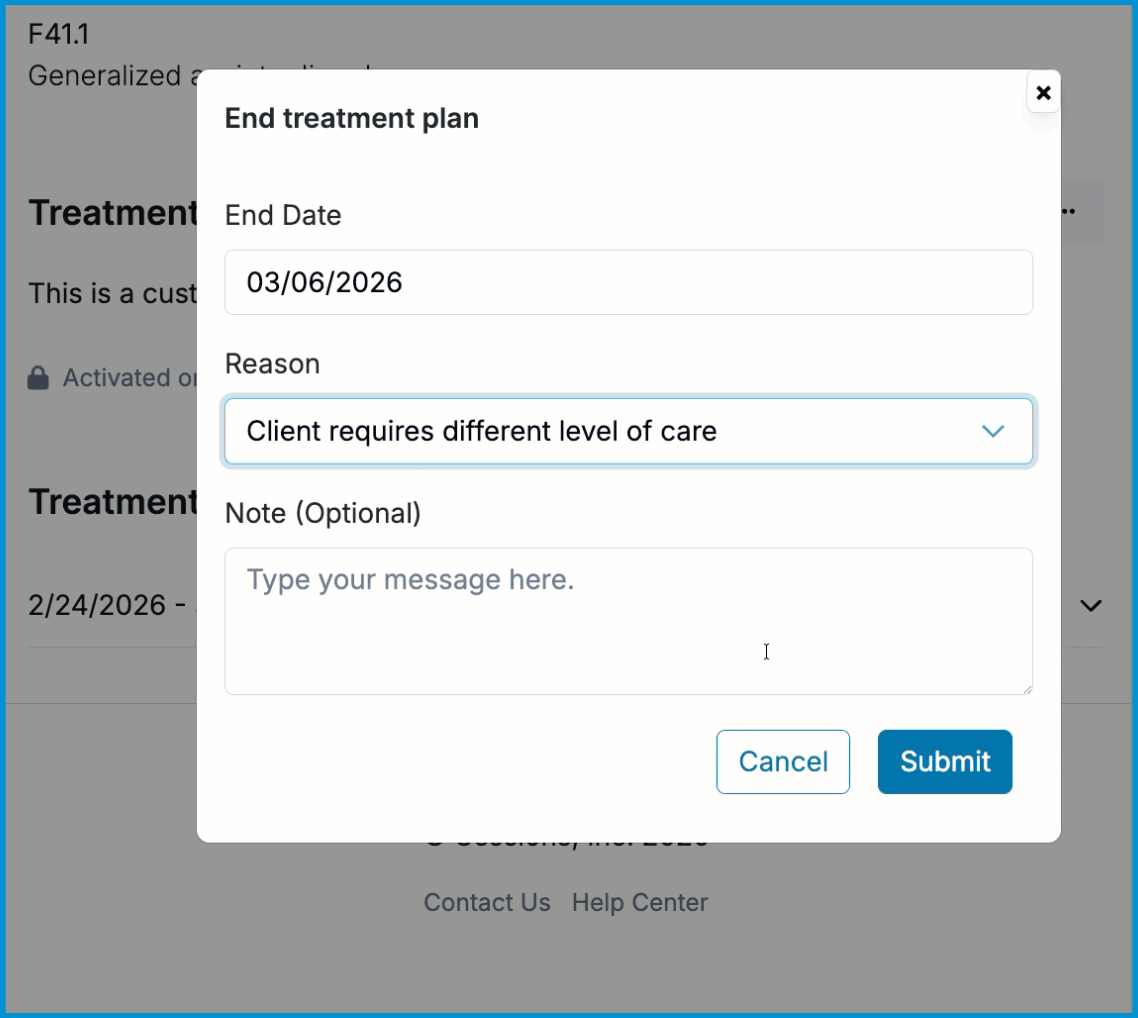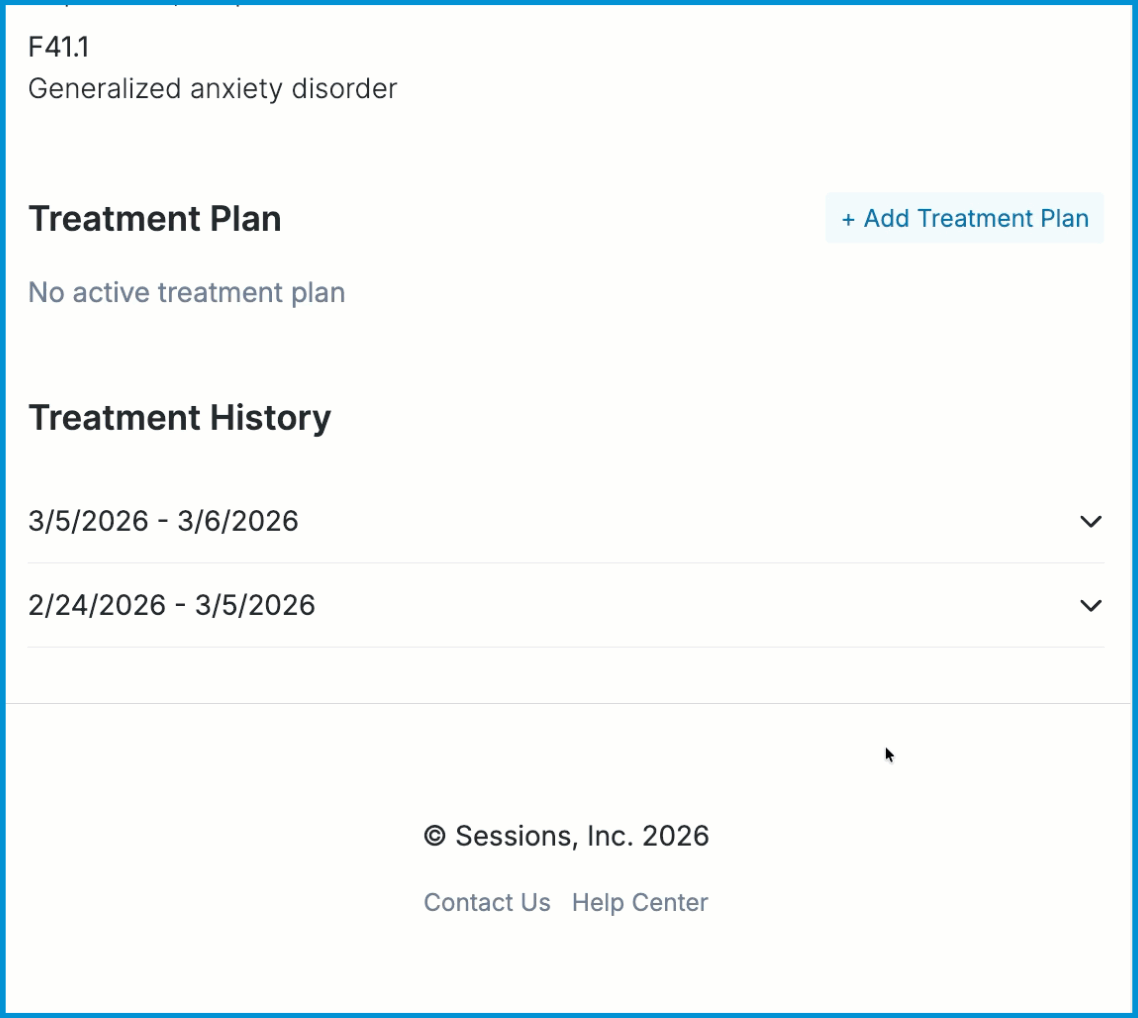
Ending a Treatment Plan
When treatment is complete or when you need to formally close a plan, you can end an active treatment plan from the three‑dot menu. Selecting End Treatment Plan opens a brief form where you can choose a preset reason for ending care and add any relevant clinical details. Once you save, the plan is marked as ended and remains available for review, audit, and reporting.
Downloading or Deleting a Treatment Plan
Once your Treatment Plan is active, you can click the "..." menu to Download a PDF of the treatment plan. From the same menu, you can select Remove if the treatment plan is no longer needed. If you wish to reuse elements of the treatment plan that are no longer needed, click the New button before removing the active treatment plan to preserve the current content.
💡 For conjoint clients, you will add the diagnosis and treatment plan in the chart for the conjoint client.
Recording Progress Towards Objectives
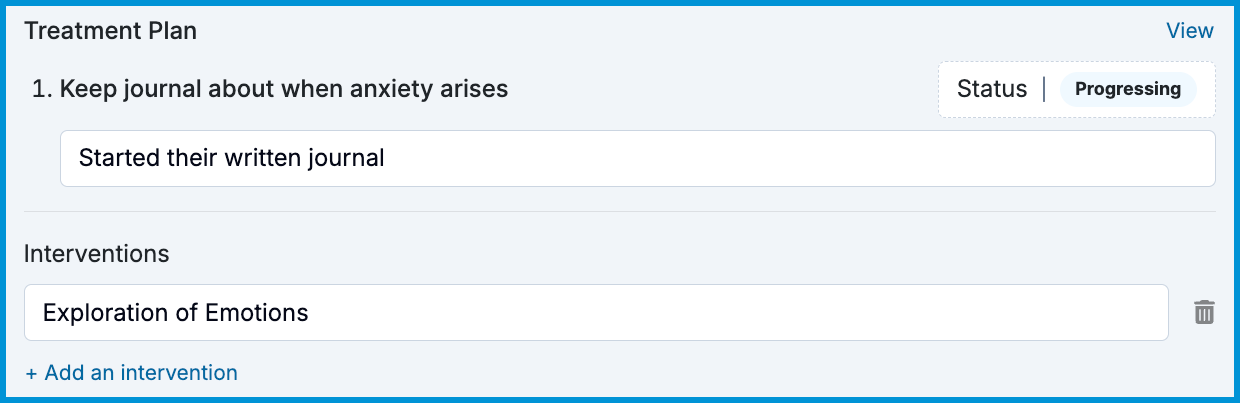
Once a treatment plan is activated, if you used the Default template or a custom template with integrated goals and objectives, the objectives will appear when completing a client’s progress note for each appointment. You may record the status of the objectives, write additional details, and list any applicable interventions in the Treatment Plan section within your note.
Updating a Treatment Plan
To update a treatment plan, click the New button.
The currently active treatment plan will be pre-loaded for you to edit, and when finished, you can Sign & Activate or Save as a Draft. Once the draft is saved, it will appear like below. You can click on the pencil icon to continue with your draft.

Once the treatment plan is signed and activated, the past version will appear under the Treatment History section.
To view the past treatment plan, click the down arrow to the right of the date duration. When viewing the previous treatment plan, you can also share, download, or remove the plan through the icons in the bottom-right corner.
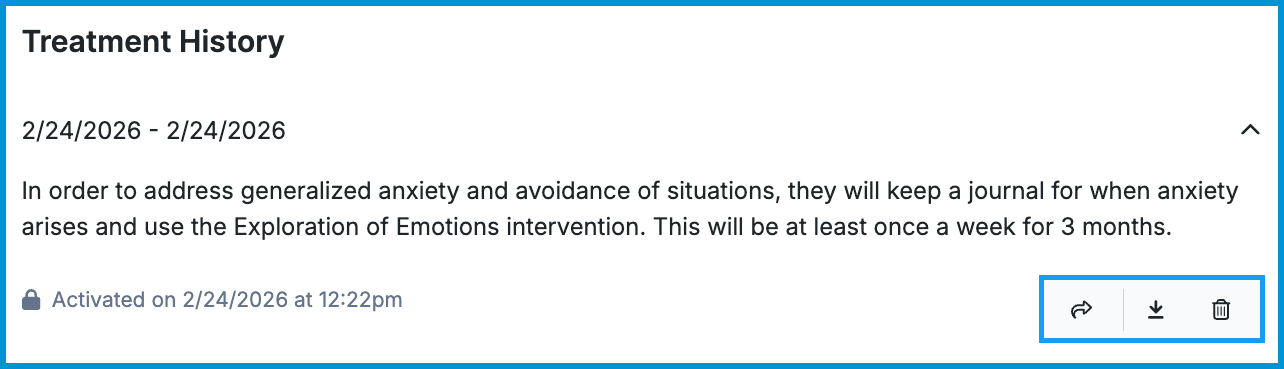
ℹ️ You can only share treatment plans with clients who have been invited to the Client Portal.
ICD-10 and DSM-V
Sessions Health uses ICD-10 codes and descriptors in our system. Since ICD-10 is currently the standard for medical billing, we adopted ICD-10.
Critiques of ICD-10
Just like with DSM-V, there are critiques of ICD-10. Some practitioners don't prefer some of the descriptions. Some don't like that it is part of a "medical model." We don't have control over the content of ICD-10 and believe it's best to use the content in a standard way. We do allow practitioners to override descriptions so that they may use their own. We don't require diagnosis or treatment plans on client charts and so for those who don't like ICD-10 for being a medical model of treatment, those parts of the system are optional. When ICD-11 becomes the standard for medical billing in the United States, we will update our system to ICD-11.
FAQ
Do you offer Wiley Treatment Planner?
Not at this time, but we may offer something similar in the future.
Why doesn't my treatment plan show up in the client's progress notes?
A treatment must be activated and include objectives in order to record the status and interventions in your progress notes. Treatment plans that are activated after a progress note is locked will appear in subsequent session notes that have not yet been completed.
Do you provide drop-downs of Mental Health ICD diagnoses to choose from?
When assigning a diagnosis, we have an auto-suggest dropdown of ICD codes available. Our system strictly uses ICD-10 codes and descriptors.
Can clients be sent treatment plans to electronically sign?
Yes. Please see Sharing Treatment Plans With Clients for more details.
How do I print notes, treatment plans, etc.?
Notes, treatment plans and other important documents are easily downloaded in PDF format to print. To download a document, click the '...' menu on any document that supports downloading. Click Download to download a PDF for printing.